A bone hormone may reverse chronic back pain in the spine, a Johns Hopkins study finds
Chronic back pain is often associated with deterioration of spinal discs and spinal end plates, which are thin layers of tissue that separate discs from vertebrae, according to medical sources.
When these elements break down, they become porous, allowing nerves that would normally not be affected to enter the center of the spine, resulting in frequent discomfort.
Research conducted by Dr. Janet L. Crane at Johns Hopkins University found that parathyroid hormone (PTH) can prevent and even reverse the growth of pain-sensitive nerves in damaged areas of the spine.
Parathyroid glands Naturally producing the hormone PTH, which experts say plays a key role in regulating calcium levels and bone remodeling.

Research suggests that thyroid hormone can inhibit the growth of pain-sensing nerves in damaged areas of the spine. (Istock)
These findings could shift the focus Back pain treatment From managing symptoms to modifying the underlying problem, according to scientists.
“During spinal degeneration, nerves that sense pain grow in areas where they normally would not be,” Crane said in a press release. “Our findings show that thyroid hormone can reverse this process by activating the natural signals that push these nerves away.”
Hidden signs your bones may be weaker than you think, according to your doctor
Synthetic versions of PTH are already used to treat osteoporosis. Previous research has suggested that these treatments may also reduce bone-related, but underlying, pain Biological mechanism It was not well understood.
Click here to subscribe to our health newsletter
Using animal models, Johns Hopkins researchers found that PTH treatment for one or two months resulted in denser, more stable vertebral endplates.
Importantly, the treatment stimulated bone-building cells, known as osteocytes, to produce a protein called Slit3, the study showed.
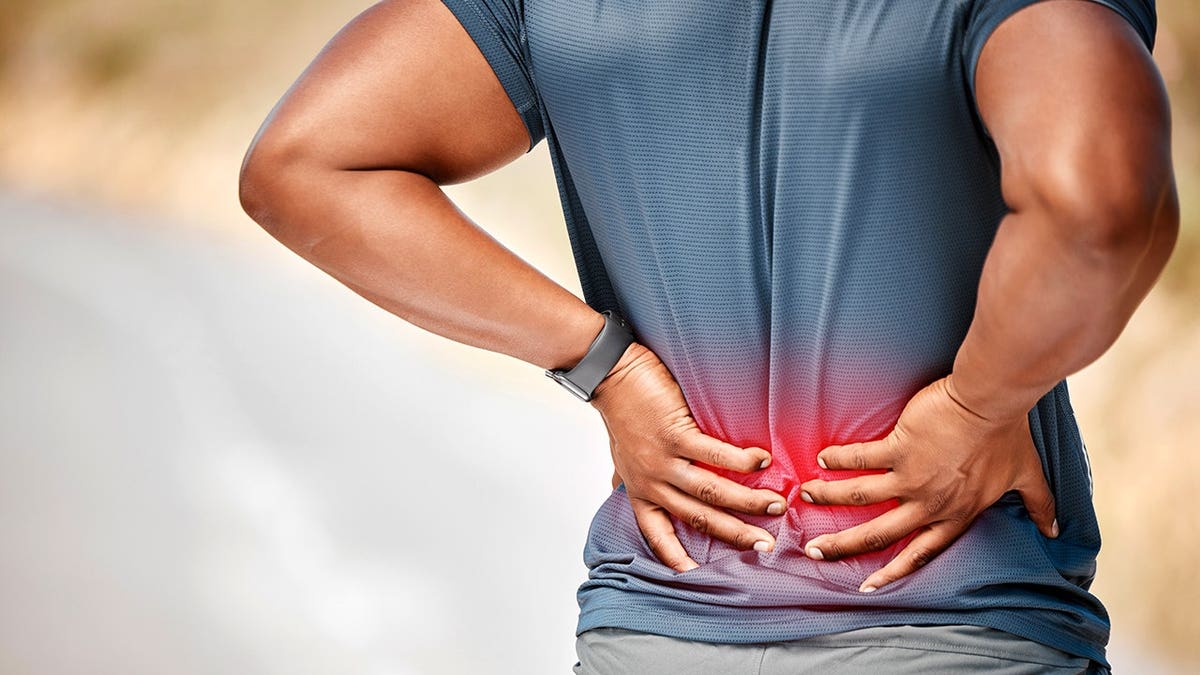
Scientists say these findings could shift the focus of back pain treatment from managing symptoms to modifying the underlying problem. (Istock)
The study found that this protein repels growing nerve fibers and prevents them from infiltrating sensitive areas of the spine.
When the researchers removed Slit3 from mice, the hormone’s pain-relieving effects disappeared, confirming the protein’s crucial role in this process.
Click here for more health stories
PTH is It has already been approved By the Food and Drug Administration for the treatment of osteoporosis. Some patients receiving bone density hormone have reported unexpected relief from back pain, a phenomenon this study can help explain.
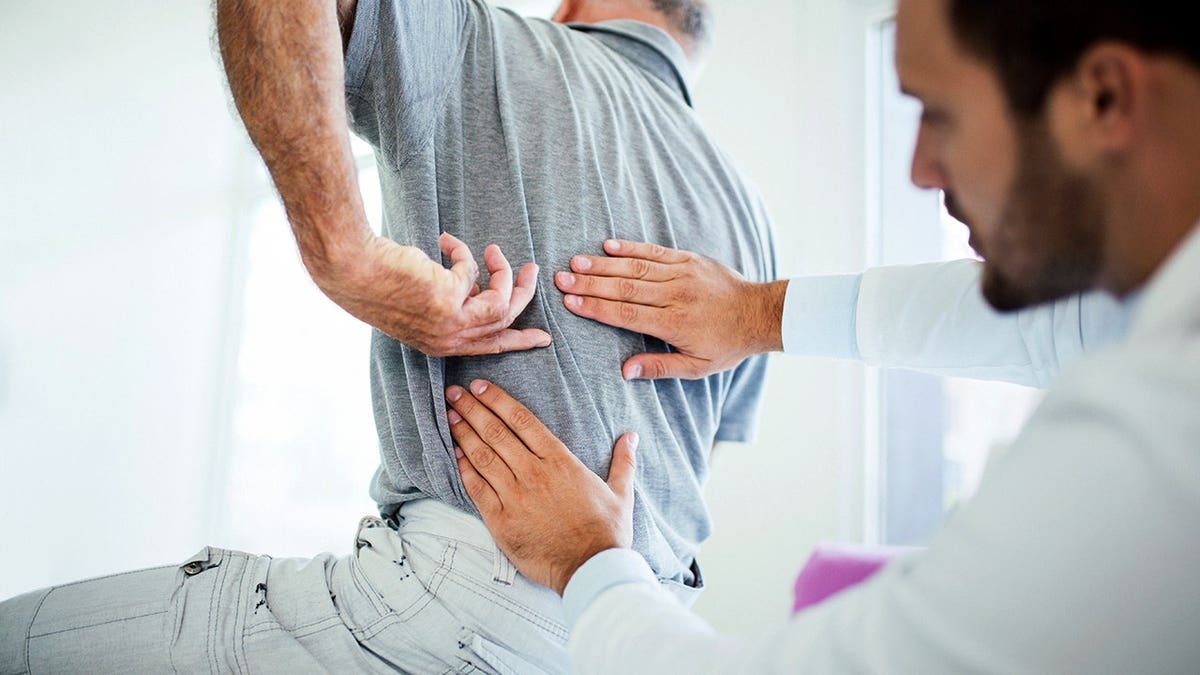
The researchers say this study lays the foundation for future clinical trials to explore the effectiveness of PTH as a disease-modifying treatment and pain relief for spinal degeneration. (Istock)
“Our study suggests that thyroid hormone treatment (low back pain) during spinal degeneration may reduce aberrant denervation (abnormal nerve growth),” Crane concluded.
The doctor said that this research lays the foundation for future clinical trials that will explore the effectiveness of PTH as a disease-modifying agent Pain relief treatment For spinal atrophy.
Click here to download the FOX NEWS app
The researchers note several limitations, including the possibility that PTH treatment may affect… Central nervous system In ways that were not fully explored in this study.
Because the study focused specifically on the Slit3 protein, more research is needed to determine how other genetic factors and bone formation processes influence spinal nerve development and pain relief.
Test yourself with our latest lifestyle quiz
The study was published in the Journal of Orthopedic Research.












Post Comment